Regulation of Extracellular Fluid Composition & Volume

Introduction
This chapter is a review of the major homeostatic mechanisms that operate, primarily through the kidneys and the lungs, to maintain the tonicity, volume, and specific ionic composition of the extracellular fluid (ECF). The interstitial portion of this fluid is the fluid environment of the cells, and life depends upon the constancy.
Defense of tonicity
The defense of the tonicity of the ECF is primarily the function of the vasopressin-secreting and thirst mechanisms. The total body osmolality is directly proportional to the total body sodium plus the total body potassium divided by the total body water, so changes in the osmolality of the body fluids occur when a disproportion exists between the amount of these electrolytes and the amount of water ingested or lost from the body. When the effective osmotic pressure of the plasma rises, vasopressin secretion is increased and the thirst mechanism is stimulated; water is retained in the body, diluting the hypertonic plasma; and water intake is increased.
Effects of vasopressin
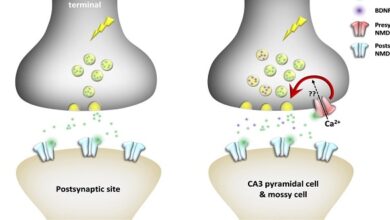
Because one of its principal physiologic effects is the retention of water by the kidney, vasopressin is often called the antidiuretic hormone (ADH). It increases the permeability of the collecting ducts of the kidney, so that water enters the hypertonic interstitial of the renal pyramids. The urine becomes concentrated, and its volume decreases. The overall effect is therefore retention of water in excess of the solute; consequently, the effective osmotic pressure of the body fluids is decreased. In the absence of vasopressin, the urine is hypotonic to plasma, urine volume is increased, and there is a net water loss. Consequently, the osmolality of the body fluid rises
Metabolism
Circulating vasopressin is rapidly inactivated, principally in the liver and kidneys. It has a biologic half-life (time required for inactivation of half a given amount) of approximately 18 min in humans.
Control of vasopressin secretion: osmotic stimuli
Vasopressin is stored in the posterior pituitary and released into the bloodstream by impulses in the nerve fibers that contain the hormone. The factors affecting its secretion are summarized in Table 39–1. When the effective osmotic pressure of the plasma is increased above the normal 285 mOsm/kg, the rate of discharge of these neurons increases, and vasopressin secretion is increased. At 285 mOsm/kg, plasma vasopressin is at or near the limits of detection by available assays, but a further decrease probably takes place when plasma osmolality is below this level.
Volume effects on vasopressin secretion
ECF volume also affects vasopressin secretion. Vasopressin secretion is increased when ECF volume is low and decreased when ECF volume is high. There is an inverse relationship between the rate of vasopressin secretion and the rate of discharge in afferents from stretch receptors in the low and high-pressure portions of the vascular system. The low-pressure receptors are those in the great veins, right and left atria, and pulmonary vessels; the high-pressure receptors are those in the carotid sinuses and aortic arch. The exponential increases in plasma vasopressin produced by decreases in blood pressure are documented. However, the low-pressure receptors monitor the fullness of the vascular system, and moderate decreases in blood volume that decrease central venous pressure without lowering arterial pressure can also increase plasma vasopressin.
Summary
Total body osmolality is directly proportional to the total body sodium plus the total body potassium divided by the total body water. Changes in the osmolality of the body fluids occur when a disproportion exists between the amount of these electrolytes and the amount of water ingested or lost from the body.